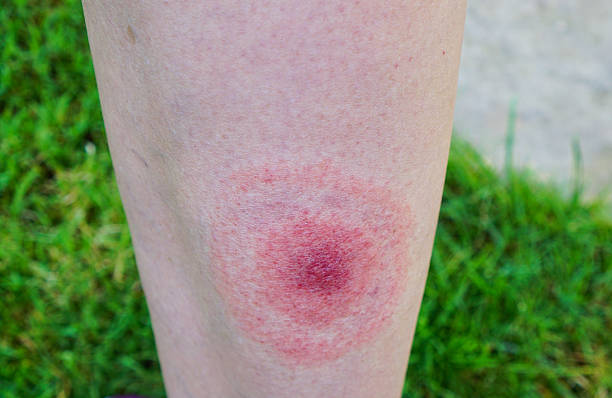
Eales disease is not synonymous with idiopathic periphlebitis. It is an inflammatory disorder that affects a subset of individuals, but not all cases are the same. Henry Eales first described it as noninflammatory, but later, Elliot described it as a form of retinal vasculitis. This condition is characterized by snowball opacities of the vitreous, neovascularization, and hemorrhage of the retina. In addition, it can lead to focal choroiditis.
VEGF
Although the exact mechanism of VEGF’s role in the development of Eales’ disease is still unclear, it appears that both pathways may be involved in the disease. A systematic metabolic disorder or permanent endothelial dysfunction are unlikely to cause the disease. VEGF is a component of the immune system, but the relationship between VEGF and eales disease remains unclear.
In the study of patients with Eales disease, researchers found a significantly increased expression of VEGF. The resulting angiogenic activity was significantly higher than in patients without the disease. Further, they found a significantly increased VEGF/PEDF ratio in patients with ED compared to those without the disease.
The pathophysiology of Eales disease is unknown but has been implicated in retinal vasculitis and neovascular glaucoma. It is characterized by a recurrent vitreous hemorrhage and is more prevalent in males than in females. A 24-year-old Indian male with a frontal headache and peripheral retinal ischemia was diagnosed. The patient underwent angiography to reveal severe retinal ischemia and vasculitis. In addition, he had a high intraocular pressure, vascular sheathing, and neovascularization in both eyes.
Treatment for Eales disease depends on the clinical stage. The mainstay of therapy is systemic corticosteroids in cases with active vasculitis. Alternatively, antituberculosis therapy is used in severe bilateral cases. However, the role of antituberculosis therapy is controversial. Some authors believe that the association between VEGF and antituberculosis therapy may be important in disease control.
IL-6
IL-6 is a type of cytokine involved in the inflammatory response to various stimuli. Its function in inflammatory diseases is unclear, but there are several potential connections between this cytokine and Eales’ disease. The disease is an idiopathic obliterative vasculitis characterized by occlusion, neovascularization, and retinal vasculitis. The disease is usually asymptomatic and inflammatory, and a diagnosis is made clinically. It is treated medically with corticosteroids, laser photocoagulation, and anti-VEGF injections.
Inflammation of the retinal veins is one of the primary causes of Eales’ disease, although this condition is also known as periphlebitis retinae. Antioxidant supplements, such as vitamin C and folate, can help neutralize harmful oxidants. These supplements can be taken on a daily basis and should be continued until homocysteine levels normalize. Several studies have reported positive results when patients receive antioxidant supplements.
In one study, the etiology of Eales disease was linked to tuberculosis, but this did not prove conclusively. Some researchers think the etiology is due to hypersensitivity to tuberculoprotein, which is a bacterial antigen. In addition, about 50-70% of patients with Eales disease were positive for at least one Mycobacterium species. In another study, a subset of patients had the MPB64 gene, which is common in tuberculosis patients. One group of researchers also noted that the MTB genome could be present in the vitreous sample of patients with Eales disease.
Studies of patients with Eales disease have shown an increased HLA phenotype, a marker of inflammatory cells. A high HLA concentration in patients with Eales disease can contribute to retinal vasculitis. It is thought that this predisposition is responsible for triggering inflammatory reactions that result in retinal vasculitis.
VEGF expression
One of the hallmarks of Eales disease is the presence of increased VEGF expression. This increased expression may explain the severity of neovascular growth and the repeated vitrous hemorrhages in the disease. However, further studies are required to clarify its exact role.
To test this hypothesis, researchers performed a study on the expression of VEGF and PEDF in eales disease. The two proteins were compared in an enucleated eye from an affected patient with the corresponding age-matched donor eye. VEGF immunostaining was found in the retinal layers surrounding blood vessels in both the Eales’ disease eye and a normal donor eyeball. PEDF was also detected in the retinal layers surrounding blood vessels in the diseased eyeball.
In both cases, VEGF and PEDF expression were increased. Moreover, the VEGF/PEDF ratio was significantly higher in PDR than in ED. The findings of these studies have implications for the treatment of this disease, which is also considered to be self-limiting.
Anti-VEGF agents have a wide range of applications. They are currently used for neovascular macular degeneration (AMD), and have also been used in 58 other eye disorders. However, there are some side effects associated with anti-VEGF therapy. While the use of anti-VEGF agents is increasing, it must be used with caution and informed consent of patients.
Treatment
The therapeutic approach in Eales disease is based on the clinical manifestations and includes systemic corticosteroids, usually oral prednisolone, opthalmological intervention, photocoagulation therapy, vitrectomy, and immunosuppressive therapy. In almost all cases, steroid therapy is associated with a dramatic response. This is consistent with the suppression of the acute inflammatory process.
The disease presents as obliterative perivasculitis affecting multiple quadrants of the retina. It is sometimes accompanied by neovascularization, uveal inflammation, or systemic disease. Diagnosis of Eales disease is by exclusion, but the Mantoux test is positive in 87% of patients.
Clinical investigation includes the following: hemogram, platelet count, renal function, HLA-B51, lysozyme, and angiotensin-converting enzyme; infectious serologic analysis; and a CT scan of the thorax. A CT reveals a cisural micronodule and a ganglion containing four microns. Several studies have also been performed to determine if systemic conditions are associated with Eales disease, including one that examined the presence of tuberculosis.
Early diagnosis and treatment are essential for the best chance of successful Eales disease treatment. Early treatment with photocoagulation can stabilize the lesions and maintain functional levels of vision. Treatment for Eales disease depends on the type and severity of the visual loss, as well as the severity of the underlying cause. The aim of the treatment is to restore vision as closely as possible.
The diagnosis of Eales disease is an exclusion procedure, meaning that other systemic diseases must be excluded. Low-grade periphlebitis is the first sign of the disease. As the disease progresses, the peripheral retinal capillaries become progressively non-perfused. In addition, the retinal capillaries may begin to neovascularize. This can cause floating spots or blurred vision.
Etiopathogenesis
The etiopathogenesis of Eales disease is poorly understood. The disease, which is more common in the Asian subcontinent, is characterized by recurrent vitreous hemorrhages. The disease affects the retina, retinal veins and retinal arteries, and it is one of the leading causes of blindness in this region. Its etiology is not fully understood, although it may involve a genetic or environmental factor.
The etiopathogenesis of Eales disease is not fully understood, but it can be attributed to three basic pathological changes. Inflammation, ischemia, and neovascularisation affect peripheral veins and arterioles, and lymphocytes are involved. Interestingly, Gilbert (1935) observed acid-fast bacilli on the perivascular sheath.
The disease has been diagnosed in young adults, and its etiology is not well understood. Various studies have been carried out to understand its cause. Although some authors report tuberculosis as a possible cause, others have reported no connection between tuberculosis and Eales’ disease.
Moreover, Eales disease is a chronic inflammatory venous occlusion affecting the peripheral retina. The disease was first described by the British ophthalmologist Henry Eales in 1880. The clinical symptoms include recurrent retinal hemorrhages, headaches, epistaxis, and chronic constipation. The disease can be treated with oral corticosteroids or laser photocoagulation.
Eales disease is a rare disorder of retinal vessels. It can lead to vascular occlusions, peripheral neovascularization, and vitreous hemorrhage. The disease usually develops in young adults.
Complications
The clinical presentation of Eales disease is characterized by obliterative perivasculitis of the retina. The colorless jelly that fills the eyeball behind the lens oozes from the retina, sometimes causing the retina to become detached. Other symptoms may include reddish discoloration of the iris and loss of vision. Additionally, cataracts may develop as the disease progresses.
Eales disease is treated using several treatment approaches, depending on the clinical stage. Treatment may include antituberculosis therapy, medical therapy, vitrectomy, and laser photocoagulation. In cases of persistent vitreous hemorrhage and bilateral vasculitis, systemic corticosteroid therapy is the mainstay of management.
One case study involved a 24-year-old Sri Lankan man who presented with acute unicular blindness. He was diagnosed with Eales disease and underwent vitrectomy and endolaser therapy to improve his vision. However, samples of the vitrectomy were not sent to a mycobacterial laboratory for mycobacterial analysis. At six months of treatment, the patient had no more recurrent vision loss. In addition, the patient also underwent chest radiography, which showed right-sided mediastinal lymphadenopathy and paratracheal lymphadenopathy. The patient did not return for follow-up.
Visual acuity in patients with Eales disease varies from normal to no light perception. However, the macula is usually spared and central vision is preserved.