How Autoimmune Disease Affects the Immune System
The prevalence of HS is 0.3-4% in the USA and Europe, with a peak incidence in the second and third decades of life. Females are three times more likely to be affected than males. Its cause is still unknown. Although the disease is not considered contagious, HS affects the immune system in various ways.
Is HS considered an autoimmune disease?
Autoinflammatory diseases are conditions where your body’s immune system mistakenly attacks its own tissues. Some of these conditions include rheumatoid arthritis, in which the body attacks its own joints. While it’s possible that HS is an autoimmune disease, researchers aren’t sure.
While HS is often thought of as a separate autoimmune disease, it often coexists with spondyloarthritis, which is another autoimmune disease. The two diseases have similar etiology and are thought to share auto-antigens. However, the presence of an autoimmune disorder does not necessarily impact treatment strategies.
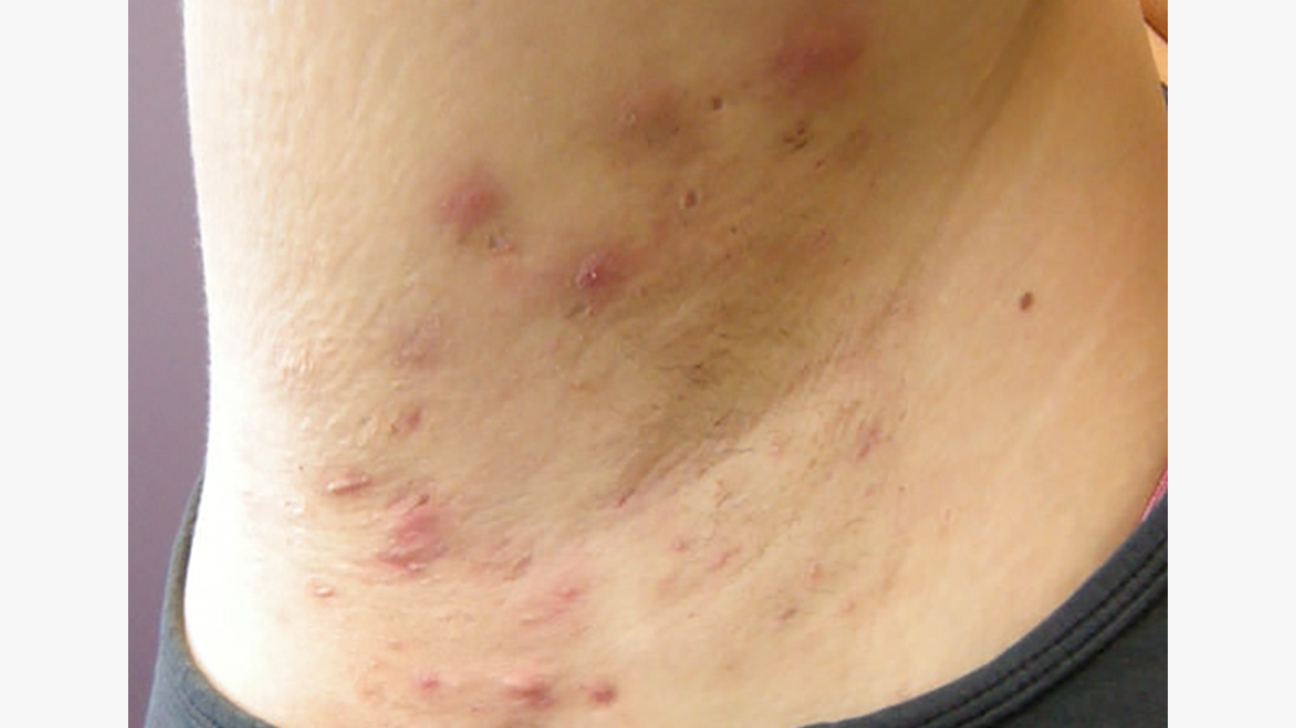
Hidradenitis suppurativa (HS) is an inflammatory condition affecting the sweat glands and sebaceous glands. This condition causes the development of cysts and abscesses, which can lead to pain and discomfort. Surgical removal of the cysts or intervention to drain them is sometimes necessary.
The causes of HS are unknown, although some risk factors have been identified. Cigarette smoking, excess weight, and family history all have been associated with the condition. Women and young adults are most likely to develop HS than men. The disease is also more common among black people in the United States than among white people.
Does HS affect your immune system?
Many people are confused about the relationship between HS and the immune system. It’s important to understand the differences between these two conditions. An autoimmune reaction is a process where antibodies in the body go rogue and attack healthy cells. This results in inflammation and tissue destruction. Research into the relationship between HS and the immune system has shown that patients with HS have elevated levels of certain antibodies. But there is no conclusive evidence that these antibodies are responsible for the inflammation.
The immune system plays an important role in the process of disease progression. People with HS have an overactive immune system, even though they may think their immune system is underactive. The inflammation is what causes lesions, which contain cells and proteins that fight infection. When the immune system doesn’t shut down properly, this causes lesions to last for long periods of time and keep coming back.
The bacteria present on the skin cause the inflammation. This inflammation causes skin cells to stick together inside the hair follicle. As a result, the opening to the hair follicle becomes blocked. This results in the formation of a thick scar, which may affect a person’s ability to walk or move their arms. Early treatment is essential to prevent scarring. If a scar is severe, a surgeon may need to remove it.
What is the root cause of HS?
When an individual has an autoimmune disease, their immune system reacts abnormally, attacking the body’s own tissues. This happens when the immune system mistakenly perceives a foreign substance as an enemy, or “self” – something it is not familiar with. For example, a person’s immune system may react to gluten, a dairy protein, or an inflammatory situation in their digestive system (leaky gut). As a result, the immune system responds abnormally, attacking the body’s tissues.
While conventional medicine attempts to suppress inflammation, functional medicine focuses on targeting the cause of inflammation. The former aims to cure the symptoms and stop the disease’s progression, while the latter aims to prevent it altogether. Inflammation is the common thread in autoimmune diseases, which are linked by a systemic, runaway immune response. The autoimmune response causes the body to attack itself and attacks healthy tissues.
Identifying the root cause of autoimmune disease is often difficult. However, it is not impossible to reverse its symptoms. Using diet and lifestyle modifications can help a person cope with the symptoms of autoimmune disease.
Can you permanently get rid of HS?
There are various treatments available for HS, including surgery and topical medications. These treatments are relatively expensive and can cause additional health risks. Wide excision, for example, is a more aggressive procedure that involves general anesthesia and hospitalization. Most health insurance policies will cover the cost of surgery. However, there are risks associated with surgery, such as bleeding and infection. Also, HS can recur after surgery. This type of treatment also leaves large scars and can damage blood vessels and nerves.
The cause of HS is not yet known, but some studies suggest that it is triggered by defective hair follicles. When this happens, inflammation occurs around the hair follicles. This inflammation causes the follicle to break open and release the hair shaft and normal bacteria. This in turn causes more inflammation. Eventually, inflammation leads to pus-filled nodules that look like boils.
While antibiotics and pain relievers can help manage symptoms, surgery can remove large lumps. Surgery is usually recommended for people with stage 2 or 3 of HS and for those with a lot of lumps. Various surgical procedures are available to treat HS, though there is not much research on which one is best for people with this condition.
Can HS ever go away?
Treatments for HS can include hormonal therapy and biologic drugs that work on the immune system. They can be administered by injections in the affected area or via IV in a vein in a clinic or hospital. These medications are approved by the FDA but can cause side effects. Some patients find that these medications help control their symptoms.
Autoimmune diseases happen when the body’s antibodies mistakenly attack a part of the body. A prime example of this is rheumatoid arthritis, where the body attacks its own joints. It’s unclear whether HS is an autoimmune disease, but researchers are looking into it. People with HS are at greater risk if they have a blood relative who has the disease, but many people who have it don’t have a family history of the disease.
Genetics are another factor that can contribute to the development of HS. Although the exact cause is unknown, it is believed that cigarette smoking increases the risk of developing HS. Being overweight can also cause HS to worsen. However, the triggers differ from person to person. Research shows that HS is more common in women than in men.
What is the life expectancy of HS?
Hidradenitis suppurativa (HS) is a chronic inflammatory disease that affects approximately 1% of the population. Symptoms include painful bumps under the skin near the roots of the hair. They can be infected and lead to scarring. In addition, HS is associated with spondyloarthritis and metabolic alterations, both of which increase the risk of cardiovascular disease.
Researchers don’t know exactly why some people develop HS. However, some risk factors include having a family history of heart disease, cigarette smoking, and excess weight. Additionally, individuals with HS are more likely to be women than men, and they are more likely to develop the disease in their early 20s and 30s. HS is also disproportionately common in Black people in the United States, and experts speculate that race may be a contributing factor.
HS diagnosis is often delayed. Patients with HS typically begin symptoms at an age of around seven years old, and it is not unusual for them to experience a number of health problems between their onset and diagnosis. Delays in diagnosis have been linked with poorer health status and a decreased quality of life.
What are the 4 stages of HS?
HS is a chronic inflammatory skin disease caused by an overactive immune system. Its early symptoms include bumps, nodules, and abscesses. As the disease worsens, it can lead to scarring on the skin. Patients may experience pain and swelling, and treatment will depend on the severity of the condition.
Researchers believe that HS is caused by an autoinflammatory reaction. It occurs when immune cells mistakenly produce cytokines, which alert the rest of the body to the presence of an invader. As a result, the body’s innate immune cells begin producing immune cells.
Although there are no exact answers for the causes of HS, it is known that one in 100 people is affected. It typically develops in the teenage or early adult years. While it is more common in women, men can also be affected. There is no known way to prevent the development of HS, but it does tend to run in families. People with HS typically begin experiencing symptoms during their early adolescence or early adulthood, and the condition rarely progresses past the age of 55.